Poster Title: Qualitative Interviews of the Lived Care Transition Experiences of Patients with COPD over the Age of 65
Organization or Hospital: White Plains Hospital
Authors:
Judy Badia, DNP, MSN, RNC, CPXP, CPPS, Clinical Nurse Scientist, White Plains Hospital, White Plains, NY
Nicolette McPartland, BSN, RN, Clinical Nurse PCU, White Plains Hospital, White Plains, NY
Debbie Pierce, RRT, PCM, COPD Transitional Care Manager, Respiratory Therapy Department, White Plains Hospital, White Plains, NY

Project Summary:
Aim: Explore patient perceptions of lived transition in care experiences and gather insights to help health care teams improve care transitions in this population.
Background: Chronic obstructive pulmonary disease (COPD) is the third leading cause of death with those diagnoses expected to rise, creating a substantial burden. COPD management is complex, often involving comorbidities, fluctuating symptoms, and the need for long-term care. The disease significantly impacts a patient’s quality of life, imposing a considerable symptom burden, both physiologically and psychologically. COPD also comes with a financial burden due to treatment costs and quality of life issues for the family or care partner.
Project Design: Critical care nurses completed Professional Quality of Life surveys (ProQOL 5) (Stamm, 2010) at before and two months after educational intervention that was designed to teach about CF and its self-care strategies. Comparisons of ProQOL scores which measured compassion satisfaction and CF (as burnout and secondary trauma scores) were made to determine if education interventions effectively improve compassion satisfaction and reduce CF
(significance level at p<0.05)
Methods:
A semi-structured qualitative design was employed, involving 10 patients with COPD over the age of 65.
Results:
Measured Data:
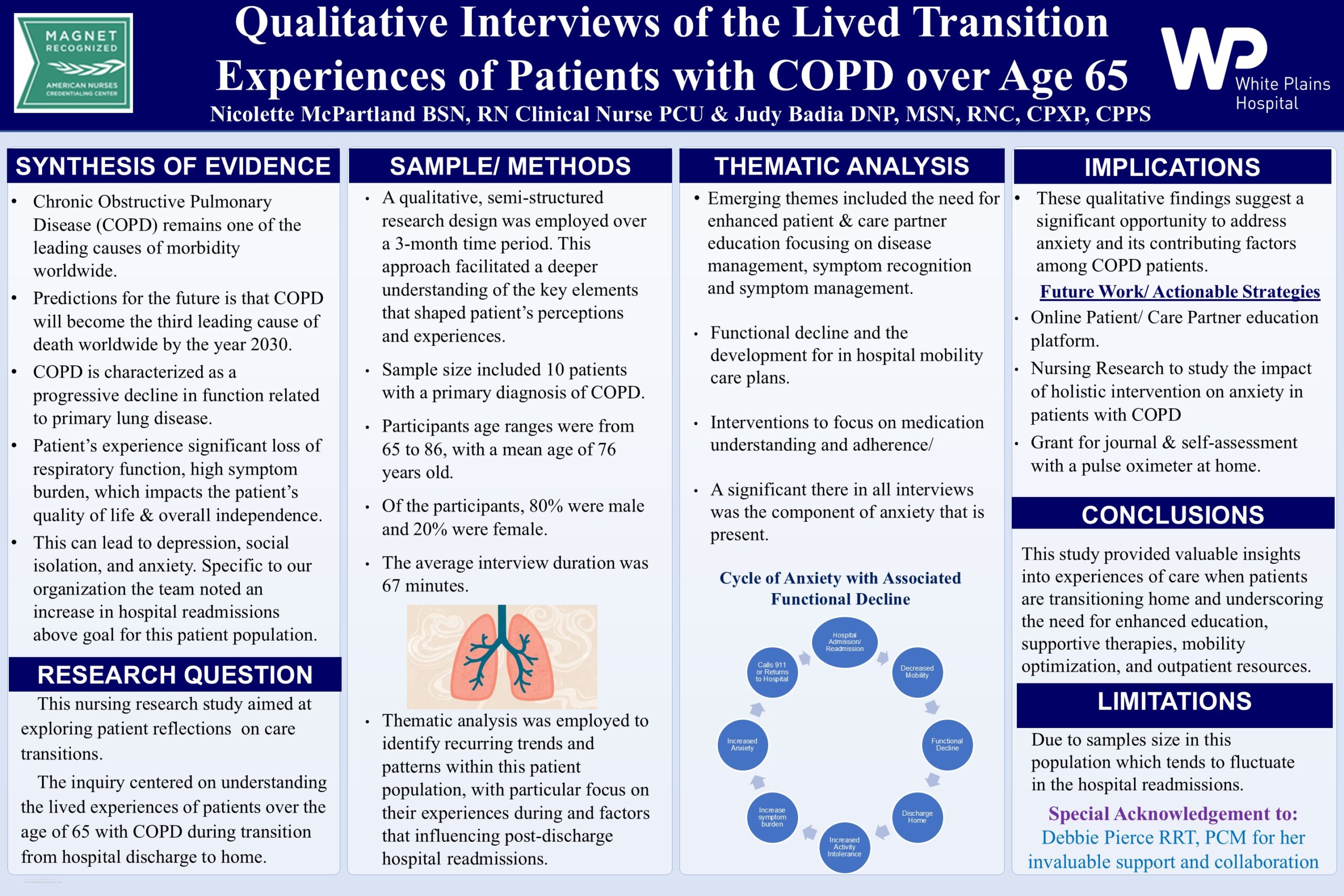
A thematic analysis was conducted that revealed a prominent theme of persistent anxiety among patients diagnosed with COPD, particularly during discharge transitions. Participants expressed feelings of security while hospitalized, comforted by the health care team’s monitoring. Upon discharge, anxiety increased due to fears of leaving the hospital and uncertainties about managing their condition at home.
Anxiety was further compounded by the complexity of COPD, as many struggled with understanding the disease and its progression. They voiced concerns about managing daily tasks like meal planning, medication, and personal care. Financial stress, particularly regarding medication costs, contributed to anxiety, with some altering their medication usage to reduce expenses, risking their health outcomes.
Participants also emphasized the need for better education on managing their condition, especially regarding environmental triggers like weather changes or illness. The lack of understanding from family and friends, coupled with social isolation, added to their stress. Participants advocated for self-monitoring and symptom evaluation, stressing the importance of including this in discharge education to improve disease management and reduce hospital readmissions.
Conclusion:
The qualitative interviews reveal the significant impact of anxiety on patients with COPD, particularly during transitions from hospitalization to home. The fear of managing their condition, combined with a lack of understanding and support, exacerbates feelings of stress and uncertainty. Participants emphasized the need for comprehensive education for both patients and their families to improve disease management and outcomes. Key strategies, such as self-monitoring and individualized discharge plans, are crucial in empowering patients to manage their health and reduce readmission risks. Addressing these concerns through targeted support, education, and improved communication could alleviate anxiety, enhance quality of life, and promote better disease management.
Building on these findings, a study is under IRB review that aims to explore the impact of a holistic approach to managing anxiety in COPD patients. Efforts are also underway to enhance online educational resources for patients, families, and caregivers, focusing on critical aspects of COPD management. Additionally, nursing staff training has been expanded, including updated inhaler use instructions and physical therapy materials in COPD patient care protocols. These initiatives aim to improve patient self-management, empower families, and enhance the overall management of COPD.
References:
Aranburu-Imatz, A., López-Carrasco, J. C., Moreno-Luque, A., Jiménez-Pastor, J. M., Valverde-León, M. D. R., Rodríguez-Cortés, F. J., Arévalo-Buitrago, P., López-Soto, P. J., & Morales-Cané, I. (2022). Nurse-led interventions in Chronic Obstructive Pulmonary Disease patients: A systematic review and meta-analysis. International Journal of Environmental Research and Public Health, 19(15), 9101. https://doi.org/10.3390/ijerph19159101
Yawn, B. P., Mintz, M. L., & Doherty, D. E. (2021). GOLD in practice: Chronic Obstructive Pulmonary Disease treatment and management in the primary care setting. International Journal of Chronic Obstructive Pulmonary Disease, 16, 289–299. https://doi.org/10.2147/COPD.S222664
Contact Person(s):
Judy Badia, DNP, MSN, RNC, CPXP, CPPS
41 East Post Road
White Plains, New York 10601
Email: jubadia@wphospital.org